
Hypertrophic Cardiomyopathy (HCM) vs. Other Heart Conditions: What You Need to Know
Understanding the Differences Matters
Many heart conditions share similar symptoms, yet their causes, risks, and treatments vary significantly. As a consequence of these similarities, misdiagnosis is common, making early and accurate diagnosis crucial for effective management and long-term heart health. Let’s explore what makes hypertrophic cardiomyopathy (HCM) unique and why recognizing it early can make all the difference.
What is Hypertrophic Cardiomyopathy (HCM)
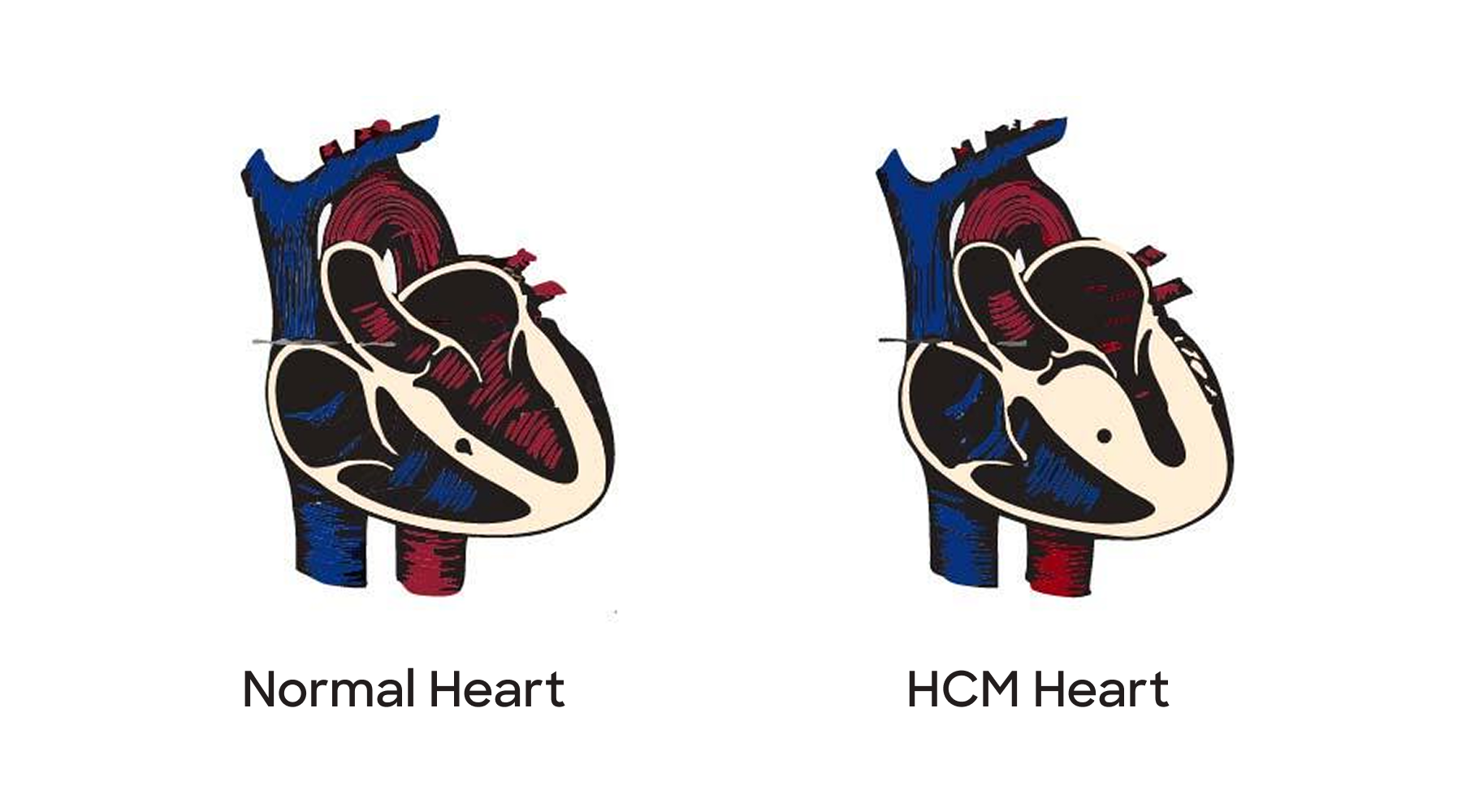
HCM is a genetic heart condition in which the heart muscle, most commonly the left ventricle, thickens abnormally. This thickening can make it harder for the heart to pump blood efficiently, potentially leading to complications such as arrhythmias or obstruction of blood flow. Unlike many other heart conditions, HCM is not caused by high blood pressure, lifestyle factors, or coronary artery disease—it’s inherited.
According to the International HCM Summit 2024, approximately 260,000 people in the U.S. are diagnosed with HCM each year. However, as many as 700,000 may have the condition without knowing it. That means HCM is more common than many people realize, possibly even more prevalent than well-known conditions like multiple sclerosis or cystic fibrosis.
How HCM Differs from Other Heart Conditions
Most heart conditions, such as coronary artery disease (CAD), congestive heart failure (CHF), or dilated cardiomyopathy (DCM), develop over time due to factors like aging, lifestyle, or underlying health conditions. They often involve problems with blood flow, weakened heart muscles, or structural damage. HCM, on the other hand, is fundamentally different—it’s a genetic muscle disorder, whereas many other heart conditions develop due to a mix of lifestyle, aging, or other health factors.
Here’s how HCM compares to other common heart conditions:
- Hypertrophic Cardiomyopathy (HCM): A genetic condition in which the heart muscle thickens abnormally, making it harder for the heart to pump blood efficiently. This can lead to shortness of breath, dizziness, and, in severe cases, sudden cardiac arrest.
- Coronary Artery Disease (CAD): A blood vessel disorder where plaque buildup restricts blood flow, increasing the risk of chest pain, heart attacks, and reduced oxygen supply to the heart. Lifestyle factors like diet, smoking, and high cholesterol are major contributors.
- Dilated Cardiomyopathy (DCM): A heart muscle disorder where the heart weakens and enlarges, struggling to pump blood effectively. This can cause fatigue, swelling, and irregular heartbeats. DCM can be caused by genetic factors, infections, excessive alcohol use, high blood pressure, or certain medications. Unlike HCM, the heart muscle in DCM becomes stretched and thin, not thickened.
- Congestive Heart Failure (CHF): A condition where the heart can’t pump blood efficiently, leading to fluid buildup, swelling, and shortness of breath. CHF is often the result of long-term damage from other conditions like CAD, high blood pressure, or previous heart attacks.
- Restrictive Cardiomyopathy (RCM): A heart muscle disorder where the heart becomes stiff, making it difficult to fill with blood properly. This results in poor circulation, fatigue, and swelling. RCM is often caused by genetic mutations or conditions like amyloidosis, sarcoidosis, and iron overload. Unlike HCM, the heart muscle in RCM doesn’t thicken—it loses flexibility.
These key differences affect diagnosis, treatment, and your heart health management strategies.
Why Early Detection of HCM is Crucial
According to the American College of Cardiology study, many people with HCM remain undiagnosed, as symptoms can be mild or mistaken for other conditions like asthma or anxiety. In fact, the study reports that more than 35% of patients either receive an incorrect diagnosis or remain undiagnosed. Without proper diagnosis, the condition can silently progress, increasing the risk of complications such as heart failure or sudden cardiac arrest.
Here’s why early detection is vital:
- It’s genetic: If you have HCM, your family members may be at risk too. Genetic screening can help with early detection and prevention.
- It’s often silent: Some people have no symptoms, while others experience dizziness, fatigue, or fainting. Recognizing warning signs early can prevent serious complications.
- It requires specialized care: Standard treatments for other heart conditions, such as certain medications, may not be safe for HCM patients.
- It can save lives: With early detection and proper management, the risks of sudden cardiac arrest and other severe outcomes can be significantly reduced.
If HCM is caught early, patients can take proactive steps to manage their heart health effectively—ensuring better long-term outcomes.
What Should You Do Next?
If you or someone you love has been diagnosed with a heart condition or if you’ve had unexplained symptoms, consider these steps:
- Consider your family history: If HCM runs in your family, genetic testing may help with early detection and prevention.
- Consult a doctor: If you’ve been diagnosed with an enlarged heart, a murmur, or unexplained fainting episodes, ask if HCM could be the cause. Since HCM is often misdiagnosed, a second opinion from a cardiologist can make all the difference.
- Understand your treatment options: Not all standard heart treatments are suitable for people with HCM. Work with a cardiologist who specializes with HCM, or other heart muscle disorders, to determine the safest and most effective approach for you.
Knowledge is Power
Heart health isn’t one-size-fits-all. HCM stands apart from other heart conditions, and understanding those differences can be lifesaving. Whether it’s you, a family member, or a friend, raising awareness about HCM can lead to better care, earlier diagnosis, and the right treatment path.
Let’s spread this knowledge. When it comes to your heart, awareness can save lives.